|
One of the biggest barriers to linking depressed and anxious new moms with the professional help they need is lack of routine screening, education and referral. This is changing in England and Australia where many hospitals already conduct perinatal depression screening programs. At Cedars-Sinai things are also changing. In April 2017 we initiated the new Postpartum Depression (PPD) Screening, Education and Referral Program. This Program received some local media attention last year, see more in my blog post from OCTOBER. With a lot of collaboration and dedication from 4 Departments across Cedars, I am thrilled to report that as of December our screening rate was 99% and remains so! Screening alone won’t help. And educating alone won’t help. Nurses, social workers & other professionals like OBGYN doctors and pediatricians must be trained to conduct the screening, education AND referral process properly. So we teamed up with Maternal mental health Now and made a PPD Screening Training video! Some of the tips for screening include:
As we prepared this training video we took into account the initial questions from Cedars nursing staff. One nurse wondered what to do in case a husband, mother-in-law or older child was in the room, “Should I go ahead and ask the questions anyways?” she asked? No – it is very important to “prepare the room” and allow a new mom to be 100% comfortable to endorse the items. Another nurse followed up by asking, “How exactly do we politely ask these family members to leave?” and “What do we say if she worries we will call child protective services if she does endorse an item?” These are all excellent and very important questions. Our training video is finished! It includes the answers to these critical questions (including limits to confidentiality) and several interviews about the protocol, including with an OBGYN doctor, a social worker and a patient representative and will GO LIVE to train the 100’s of Postpartum and Maternal Fetal Care Unit nurses at Cedars next month! Here is the first minute of the role-model segment of the training video. For the full 10 minute video please go to Maternal Mental Health NOW's website, and inquire with the Training Director, Gabrielle Kaufman if it has not yet been made available to the public.
Thanks for watching!
3 Comments
I was honored to participate in the California State Senate Health Committee Hearing in Sacramento last week where both AB 2193 (MD screening and insurer case management) and AB 3032 (Hospital Maternal Mental Health) passed and moved on to the Appropriations Committee. Our team, led by 2020 Mom and Maternal Mental Health NOW, included other maternal mental health and health providers as well as survivors (Markeyta Stocker-Sandoval pictured), family members and other advocates. I testified on behalf of Cedars-Sinai and Perinatal Mental Health Care for a very important bill to provide screening, education, referral and primarily case management for pregnant and postpartum women. This is my testimony. July 2019 UPDATE: The rule became effective on July 1, 2019
What does this bill do?
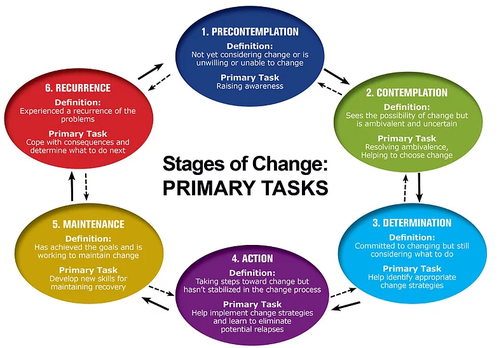
To learn more, please see Maternal Mental Health Now's Guide to Implementing the 2018 Maternal Mental Health Bills. Human beings are creatures of habit. That can be a very good thing if we have mostly healthy habits! Every one of us, however, has a bad habit like eating too much junk food, not getting enough sleep, smoking, drinking too much or never exercising. If you are thinking of getting pregnant then the time to make a change is now! I am not suggesting that changing your behaviors is easy. As you can see in the STAGES OF CHANGE image above (Prochaska & DiClemente's Trans-theoretical Model of Change), changing your behavior can take time. Believe me, I have struggled to make behavior changes throughout my life and the process can be long and hard. Lets take my smoking addiction as an example: STAGE 1: I was a cigarette smoker for 15 years (5 of those years I was a heavy smoker, 1-2 packs a day) and quit exactly 15 years ago! I loved smoking and certainly didn't quit overnight. First, I had to do some deep soul searching to understand WHY I was still smoking after all those years. STAGE 2: I mistakenly thought that smoking brought stress reduction. I had used smoking as a "break" from studying - in high school, college and grad school. I felt that I worked hard and deserved this one thing to help calm me down. But I also noticed that I felt revved up after smoking too much (which I often did) and that I was smoking at other times too - when I went out with friends, when I had a cup of coffee (major trigger for me), etc. If I didn't smoke (long plane ride) I had a huge headache. I knew it was bad for my lungs, my heart, my skin etc. And once my nephew was born I wanted to be around him without smelling like an ashtray and exposing him to any pollutants. That was the last straw. STAGE 3: I became determined to cut down. I was in grad school and started reading about how to quit smoking and was being trained in Motivational Interviewing, a highly effective therapy that I currently use with my patients who are motivated to make behavior changes. STAGE 4: I restricted my smoking to a certain number of cigarettes per day. I went slow, because that worked for me, but for others cold-turkey may be the way to go. After 1 year I had cut down to only 10 cigarettes a day. After 2 years I was down to 5 cigarettes and by the time I met my husband, when I was 27 years old, I was only smoking 1-2 cigarettes a day! So when he encouraged me to quit, I was ready! STAGE 5: I had to be vigilant at first to maintain this new lifestyle and unfortunately there was collateral damage. I had to stop being friends with an entire group of wonderful people because I knew I couldn't be around them and not smoke. It wasn't their fault, but I had to stay focused and maintain my new healthy habits. I started exercising more and eating right - and that helped me manage stress WAY better than smoking ever did! Recurrence/Relapse: Don't beat yourself up if you don't stick with your plan 100%. I crave cigarettes often, even 15 years after quitting! It's never too late to cut down or quit smoking. The benefits kick in immediately and at any age one can extend your life and improve your health! A study in the April 2005 Annals of Epidemiology reported that women who quit before age 30 are no more likely to die from lung cancer than their counterparts who never smoked. Read more HERE.
You may need professional help to achieve your goal (whether its smoking or any other unhealthy behavior), and that is ok. We are here for you! May is Maternal Mental Health Awareness Month and we are kicking it off today - Its so important that we need an extra day in April to get ready for all of the events, programs and awareness campaigns! This year Perinatal Mental Health Care has teamed up with the Maternal Mental Health Coalition of Ventura County (MMHCVC) and the Blue Dot Project. The Blue Dot is the national symbol for maternal mental health survivor-ship, support, and solidarity. We will be posting every day this week on Facebook and Instagram about maternal mental health to encourage new moms to speak honestly about motherhood, without shame, and to feel comfortable to reach out for help! Day 1 - Monday April 30th, 2018 - AWARENESS If you live in the Los Angeles area, please join the MMHCVC Motherhood Color Walk on Saturday May 19 at 10 am at the Promenade Park in Ventura, CA. The MMHCVC was established in 2017 as a non-profit, volunteer, public and private network dedicated to promoting maternal mental health and wellness through education, advocacy, assessment, treatment and training. Join us as we walk to raise awareness and funds to support moms and families by advocating for Maternal Mental Health! UPDATE: We raised ALMOST $2500 of our $3000 goal on the 19th. Please click HERE for information about how YOU can still help!!! Even after the event - we hope to reach our goal and serve women all over Ventura County, CA and beyond! Day 2 - Tuesday May 1st, 2018 - RESEARCH Perinatal Mood and Anxiety Disorders (PMADs) affect the mother, her fetus/newborn (adverse perinatal outcomes), her partner, older children, extended family and in many cases (e.g. when she cannot return to work because of her symptoms) society as a whole. In addition to treating women with PMADs I am committed to understanding WHY some women develop these problems and also what the consequences are. I was honored to be invited to submit a paper to the Journal of Behavioral Medicine's Special issue on PMADs. The paper is focused on 2 risk factors for adverse perinatal outcomes (APO; like preeclampsia, preterm birth etc.), prenatal vitamin d deficiency and prenatal depressive symptoms. Having both risk factors placed women at the highest risk for APO! If you would like to read more click HERE. DAY 3 - Wednesday May 2nd 2018 - GLOBAL MISSION Its World Maternal Mental Health Awareness Day! Worldwide, as many as 1 out of 5 women are suffering with perinatal mood and anxiety disorders! The exact statistics vary by country, but its clear that families of all backgrounds are in need. Read more HERE. DAY 4 - Thursday May 3rd, 2018 - CLINICAL CHANGE In April of 2017 I helped initiate a new Postpartum Depression Screening, Education and Referral Program in the Postpartum and Maternal Fetal Care Units as part of my role at Cedars-Sinai. This Program received some local media attention last year, see more in my blog post from OCTOBER. With a lot of collaboration and dedication from 4 Departments across Cedars, I am thrilled to report that as of December our screening rate was 99%! More information will be shared about this Program in the coming months. More recently, I was honored to be interviewed for Cedars-Sinai's blog post about postpartum mood and anxiety disorders! Please click HERE to learn FIVE things about postpartum depression that you may not know! DAY 5 - Friday May 4th, 2018 - EDUCATION One thing I especially love about my career is that I get to educate people about perinatal mood and anxiety disorders (PMADs). In honor of Maternal Mental Health Awareness week, I was invited to 2 different Intensive Care Unit meetings at Cedars-Sinai to educate nurses, doctors and other staff about PMADs. The Neonatal ICU (NICU) and Maternal-Fetal CU (MFCU) staff understands that women with perinatal complications and those whose babies have medical complications are at even HIGHER risk for PMADs! The rate jumps up to 1 in 3 women! We are working hard to identify women at risk and provide the best holistic care that they need!
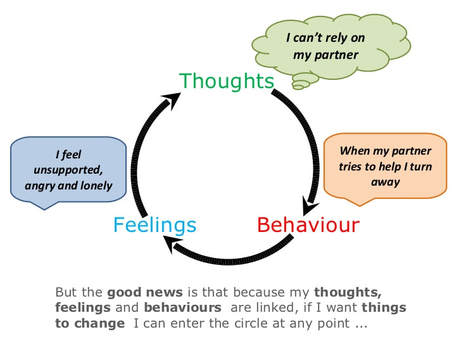
Thank you so much for your interest in this work! Again, I want to thank the organizations that we have teamed up with including Maternal Mental Health NOW (who provides our education materials at Cedars-Sinai) the Maternal Mental Health Coalition of Ventura County (MMHCVC) and the Blue Dot Project. The Blue Dot is the national symbol for maternal mental health survivor-ship, support, and solidarity!  We need you! You can easily show your support of this bill and the other 3 in the #4Bills4CAMoms package. Please read more about the bills HERE. Use 2020 Mom's letter writing web page, which takes less than 2 minutes. Add your address and with a couple of clicks a letter is emailed to your assembly member asking them to co-author all four bills. Do it now, here. Thank you for caring about the health and well-being of new mothers! Have you ever wondered what CBT is? It stands for Cognitive Behavioral Therapy, right? Ok, but have you wondered what that actually means?!? Instead of lecturing you about core beliefs, the cognitive triad, automatic thoughts, cognitive distortions and citing hundreds of research articles about how effective this therapy can be, I thought that a few images will help you understand how it works, especially for a new mom. This first image, thanks to the Parent Connection (UK), shows how our thoughts (also known as cognitions), feelings and behaviors are linked - and these arrows should be bi-directional, because in this example, feeling unsupported or lonely might also cause one to turn away from a partner or a friend. But thoughts are not facts. Let that sink in for a minute and then take a look at all of these cognitive distortions we make, many on a daily basis: So what now?? I have visually shown you how your thoughts influence your feelings and cause you to act in ways that may not help - which is probably not news to you. The slideshow of images below, thanks to a former patient (all identifying information removed), is a step-by-step example of a thought record that a new mom completed in session to begin to challenge these thoughts and change the resulting feelings and behaviors. Cognitive behavioral therapy is a process that takes 10-12 fifty minute sessions and thought records are only one piece. I am asked about how this therapy works, on a regular basis (even from the physicians I work with at Cedars), and thought this post might help.
If you have questions, please comment below and/or contact me. This weekend I went away with girlfriends to celebrate a close friend’s milestone birthday. I am so privileged and grateful to be able to afford to go on a trip like this every few years. We decided to go to Miraval, a beautiful resort outside of Tucson, Arizona. This place is the epitome of self-care and I enjoyed my weekend which included many activities like a rose renewal massage (pictured above), mindfulness meditation, yoga and hiking. This may be what many imagine is self care = too expensive and time-consuming. But that isn’t really an accurate definition.
What is self-care? Self-care is about identifying your own needs and taking steps to meet them. It is taking the time to do some of the activities that nurture you as a living breathing human being who cannot (and should not) always be on autopilot. And it is particularly important for new and expecting moms. Why? The only way I can answer that question is to tell a story. I used to fly a lot during my college and grad school years. The flight attendants always described the safety features of the plane and I got very used to ignoring this spiel. Then I had a baby. This time when the flight attendant said, “in case of a change in cabin pressure an oxygen mask will drop in front of you and you should put on your own oxygen mask before you assist anyone else,” I thought - Wait, what? I take care of myself first?!?! I decided on that very flight that I was learning something very important: Only when we first help ourselves can we effectively help others. Caring for yourself is one of the most important things you can do for yourself. It is also one of the easiest things to forget. But you benefit greatly from self care and so do others in your life. Why is Self Care Important specifically for Women? Women spend most of their lives nurturing others. This can be fulfilling and still have significant ramifications: "When we find ourselves focusing more on others than ourselves, we become worn out, stressed out and run down. For those of us who spend time helping and caring for others, it is too easy to neglect our own needs. It’s like “running on empty” when we don’t take the time to re-fuel. We spend so much time and effort caring for our partners, children, pets, friends, family members, employers and employees. Add to that the numerous volunteer activities, errands, housework, family functions, meetings, etc.—and there isn’t much time left for caring for ourselves. Women need to balance the stress and activity of daily life with activities that bring a sense of peace and well being to their minds and bodies. Women who neglect their own needs and forget to nurture themselves often become unhappy, have low self-esteem and feel resentment. Self care can help you avoid this outcome by treating yourself as a worthwhile person who is valuable, competent and deserving." *Fort Garry Women's Resource Centre What are Some Examples of Self Care Activities? Practicing self care does not have to cost a lot of money. In fact there are many things that you can do that are free or inexpensive:
My personal goal is to do one of these things for myself every single day. Sometimes I only get 10 minutes for myself. Other times I can spend an hour. But I make the time, because I am worth it and because it allows me to be the best mother, wife, psychologist, scientist, daughter, sister, friend etc. that I can be. For registration information please click HERE My program of research at Cedars-Sinai focuses on mood and anxiety disorders during the female reproductive life course and in response to chronic illness. I study the physiological processes that are associated with higher risk for depression and anxiety in pregnancy, postpartum, perimenopause, and following diagnosis and treatment of breast cancer and heart disease. I am also interested in the association between maternal mental health and adverse pregnancy and birth outcomes. My results are published in peer-reviewed journals and I strive to produce work that informs my own and others' clinical practice.
I am the primary or co-investigator on three ongoing institutional review board (IRB)-approved research studies: (1) The Postpartum Heart Health Registry and Biorepository which is designed to understand how early cardiovascular screening and evaluation can help child bearing women reduce their risk of developing heart disease later in life. This database of women with complications during pregnancy will allow us to longitudinally study possible links between complications during pregnancy, mental health, and heart health; (2) The PROVIDE study: Preeclampsia Research on Vitamin D, Inflammation, & Depression which explores whether systemic inflammation and vitamin D deficiency place women at higher risk for developing preeclampsia and postpartum depression; and (3) The Postpartum Depression Quality Improvement Study which will determine accurate prevalence rates of postpartum depression at Cedars-Sinai, test the acceptability and effectiveness of the new Depression Screening, Education and Referral program and will provide valuable patient centered qualitative and quantitative data that can be used in future services planning. In addition to the three ongoing IRB-approved research studies, I work on analyzing and writing up data collected on Vitamin D levels (not nutritional intake, blood levels) and perinatal depression and other important birth outcomes like preeclampsia and preterm birth. Some of this data will be discussed in an upcoming FREE webinar on Thursday February 1st, 2018. Session Goals: African American women have the highest rates of prenatal and postpartum depression as well as adverse perinatal outcomes (e.g. preterm delivery & low birth weight babies) compared to other racial groups in the U.S. They are at increased risk for vitamin D deficiency because darker skin limits synthesis of vitamin D and due to lower intake of supplemental vitamin D. An exciting and novel area of research focuses on vitamin D’s anti-inflammatory properties and possible anti-depressant effects. Learning Objectives: 1. Identify symptoms, prevalence and consequences of depression and anxiety in pregnancy and postpartum, with a focus on racial disparities. 2. Learn about the links between perinatal depression and vitamin D and inflammation. 3. Become familiar with research on adverse perinatal outcomes, including depression, and postpartum multi-systemic dysregulation, as measured by high allostatic load. For registration information please click HERE. My husband and I went shopping for a new mattress last weekend and it got me thinking about menopause. Why? Well, the sales woman kept talking about the Brisk mattress and winking at me. Ok, I’ll bite. I finally asked her, “What is a Brisk mattress?” She looked cautiously from me to my husband, and back again, and whispered: “You know, for the CHANGE. It’s for when you get hot at night.” Ohhhhh. Well, damn. Do I look old enough for that?!?!? Trying not to get offended, I thanked her and we moved on. Since I currently use 3 blankets to my husbands one, we laughed it off and did not buy a Brisk mattress. The interaction, however, got me thinking... Comedienne Sandra Tsing Loh jokingly says that, "Menopause isn't the "CHANGE" it's the “RETURN” to who you were before the fertility cloud came down!" Her funny TEDx talk made me think about menopause, and the psychological symptoms related to reproductive change, in a completely different way. Check it out: When I was in graduate school I reviewed the research literature on perimenopause and depression. Researchers had discovered that the risk of new-onset depression increased during the perimenopause and that sex hormones (like estrogen and progesterone) were associated with this risk. Whether depressive symptoms are directly related to changes in reproductive hormone levels is a controversial issue in women’s health. Specifically, some researchers insisted that depression in women occurs more often during times of intense hormonal fluctuation (during menstruation, postpartum, and menopause) and it is exposure to changes in hormone levels that are important - rather than absolutely low levels. In support of their theory, they note that there is a relatively low incidence of depression at times of stable hormone levels, as in the postmenopausal years. More recent research found that the earlier a woman goes through menopause, the higher her risk for depression, especially if the early menopause is due to medical reasons, i.e. cancer treatment etc. Ten years and 2 kids later, the science hasn’t changed too much. Thanks to Loh, however, my perspective on this topic has. She exaggerates to say that fertility is a relatively short period of our lives. Depending on how long you live, it could be half of your life! But the wisdom in her joke is that we can choose to perceive it as the most important half, or not. If not, then we don’t have to grieve the “CHANGE.” We may struggle at first, with the physical and emotional changes, and we may need support through those changes. But we don’t have to despair nor do we have to go through it alone. References 1. Accortt EE, Bower JE, Stanton AL, Ganz PA. Depression and vasomotor symptoms in young breast cancer survivors: the mediating role of sleep disturbance. Archives of women's mental health. 2015; 1; 18(3):565-8. 2. Cohen LS, Soares CN, Vitonis AF, Otto MW, Harlow, BL. Risk for new onset of depression during the menopausal transition. The Harvard Study of Moods and Cycles. Arch Gen Psychiatry. 2006; 63:385–390. 3. Freeman EW, Sammel MD, Lin H, Nelson DB. Associations of hormones and menopausal status with depressed mood in women with no history of depression. Arch Gen Psychiatry, 2006; 63:375–382–382. 4. Georgakis MK, Thomopoulos TP, Diamantaras AA, Kalogirou EI, Skalkidou A, Daskalopoulou SS, Petridou ET. Association of age at menopause and duration of reproductive period with depression after menopause: a systematic review and meta-analysis. JAMA psychiatry. 2016; 1; 73 (2):139-49. 5. Richardson T, Robinson R. Menopause and depression: A review of psychologic function and sex steroid neurobiology during the menopause. Primary care update. Obst Gynecol. 2000; 7: 215–223. Social support is critical at any stage in life, especially for a new mom learning the ropes. Virtual or online support is even more important and useful if that mom recently moved to a new area and hasn't yet built a support system. I was interviewed back in March about the importance of social support in mothers. The CBS reporter spent almost 30 minutes asking me many questions, yet they only ended up using about 12 seconds of my answers. That is ok, except that they left out a very important conclusion which is that IF depression or anxiety is interfering with a mother's functioning (she cannot take care of herself or her baby), then it’s time to seek professional help.
|
Dr. Accortt in the NewsAugust 2023: KPCC Radio AirTalk with Larry Mantle, FDA Approves Pill Designed To Work Faster For Postpartum Depression
August 2023: KABC TV: Postpartum depression drug aimed at prioritizing maternal health, especially in communities of color February 2023: Glamour Magazine: Postpartum Anxiety Is More Common Than You Think—Here’s What You Need to Know December 2022: Cedars-Sinai Newsroom: Immune System Irregularities Found in Women With Postpartum Mood & Anxiety Disorders October 2022: Verywell Family, Researchers Find Possible Predictor of Postpartum Depression June 2022: ABC News, Postpartum Depression Screening, Changes to Nurse Training. August 2021: AirTalk KPCC Radio, The History of C-Sections, The Significance We Put on "Birth Stories" And How It Impacts Mental health (fast forward to 13 minute mark) July 2021: AirTalk KPCC Radio, Why Women Have Long Kept Early Parts of Pregnancy a Secret and the Arguments For Moving Away From the 12-week rule (fast forward to 28 minute mark) July 2021: Los Angeles Times, Postpartum depression on the rise, especially for women of color, during COVID-19 pandemic October 2020: The Candidly, PMDD Affects Millions Of Women. So Why Aren’t We Talking About It? October 2020: Cedars-Sinai Discoveries Magazine, A Real-Life Stress Test September 2020: Cedars-Sinai Blog, Infertility and Mental Health July 2020: Cedars-Sinai Newsroom, Reproductive Psychology Program Focuses on Mother and Family Wellness May 2020: Hawaii News Now, Sunrise, How to Prevent Anxiety & Depression Before and After Giving Birth April 2020: The Bump, How to Spot Postpartum Depression in Your Partner or Friend 12/3/19: Quartz, Ten questions about mothers’ mental health could promote resilient pregnancies 5/10/19: CGTN America, US comedian uses her act to turn the spotlight on postpartum depression 5/1/19: KTLA News, How One Comedian’s Battle With Postpartum Depression Turned Laughs Into Legislation 3/20/19: KFI News Radio, FDA Approves First Drug for PPD, Brexanolone (Zulresso) Winter 2019: Cedars-Sinai Discoveries Magazine, Stop The Stigma 9/11/18: USC Center for Health Journalism, Cedars-Sinai PPD Screening Program May be Model for State Summer 2018: Cedars-Sinai Catalyst Magazine, The Helping Hand of Los Angeles Funds Postpartum Depression Screening Program, scroll down to page 40 of magazine 5/18/18: TODAY.com, Alyssa Milano on Postpartum Anxiety 5/3/18: Cedars-Sinai Maternal Mental Health Research 10/19/17: Cedars-Sinai Postpartum Depression Screening Program 3/24/17: MomCo. App for Social Support Blog Archives
May 2022
AuthorDr. Accortt is a California licensed clinical psychologist. When she isn't seeing patients in private practice she conducts research in the OBGYN department at Cedars-Sinai. She will update this page with important maternal mental health news and research. |
















 RSS Feed
RSS Feed