|
Perinatal mood and anxiety disorders (PMADs) are one of the MOST common complications of child birth and maternal suicide is one of the leading causes of maternal death. There are more new cases of mothers suffering from maternal depression each year than women diagnosed with breast cancer! More than 600K women suffered from MMH disorders in the US each year BEFORE COVID19 (rates are higher now) -- yet less than 15% of those diagnosed ever receive treatment. How can we as a community change these numbers? How can we prevent new cases and increase connection to care for the diagnosed cases? 💥Raise awareness 💥Influence policy 💥Change attitudes I kicked the month off with a press release from Cedars-Sinai highlighting our most recent quality improvement publication. Read the press release in this LINK. To read the full research study, head over to "Favorite Links" and select "Featured Research Article." To raise awareness, I was invited by Cedars to do an IG Take Over and it was a lot of fun! To follow a "Day in the Life" of a Reproductive Psychologist - go to Cedars Instagram and select the Green Highlight entitled "RPP DITL." A quick link to that can be found HERE. I was also excited to be invited to chat with Alessandra Torresani on her Emotional Support Podcast about PMADs! She has always been open about her Bipolar diagnosis and she just announced that she is pregnant for the first time! I was able to share all the facts about PPD and Al said this conversation "put me at ease during my pregnancy, not letting FEAR of the unknown take over. Bipolar Psychosis is a very real diagnosis I've read so much about and I have the opportunity to break it all down." Check out the full podcast HERE!
0 Comments
I loved this book! I am so glad I did because the author is a close personal friend of mine. Alison Ross, LMFT, is the founder of Non-Dieting Health, psychotherapy services for those who struggle with yo-yo dieting, bulimia, binge-eating disorder, anorexia, or any disordered eating state. She asked me to write a review and I am so pleased do so because I learned a lot about myself and about how some of my clients might struggle with body image. I think you will too, even if you don’t personally struggle with eating or body image. Indeed, I answered “no” to all 6 questions she poses on the back cover of her book and believe this book was STILL very much for me! I didn’t know what body image was until I started college. Before then I was aware that we all differed in appearance, but I suppose I was fairly “Body Positive.” The body positivity movement encourages you to love and feel good about your body, no matter what it looks like. Body positivity emphasizes the idea that “everyone is beautiful.” Body neutrality, on the other hand, simply proclaims that everyone “just is.” My parents raised me to believe I was beautiful. In every way. And they raised me to love to eat! My friends in middle school and high school were all beautiful and loved to eat too! We had a blast sharing each other’s ethnic foods and I was proud of my friends primarily for their personalities and their souls, not for their looks. But I noticed their external beautiful qualities and sometimes I was jealous. I wanted Koliwe’s smile, Grace’s hips, Mickey’s hair and Kimberly's legs. I didn’t realize that this jealousy could be poisonous. I didn’t realize it could cause one to feel ashamed and to “hustle” to change. I knew I wasn’t perfect, but I still felt beautiful. In high school I had another friend who lost a lot of weight very quickly and in college I made a close friend who later shared with me that she had anorexia in High School. Her stories about exercising to exhaustion and only eating one saltine an entire day reminded me of my old friend and confused and shocked me. It was late in college that I became interested in pursuing psychology and in the following decade I learned more about anorexia as well as many other mental disorders. But it wasn’t until many years after I earned my PhD in Clinical Psychology, when I befriended Alison, that I learned about yo-yo dieting and binge eating (not included in the DSM manual of mood disorders). “Food is love,” Alison writes in chapter 2 of her book. Isn’t that the truth! When I struggled to breastfeed my first child I learned how upsetting it can be to feel like a failure, to not be able to calm and nourish your very own child. My husband was patient and soothed our crying son (and me), without providing him milk and for that I was thankful. But food is indeed love. And later when my son and I got in sync and I could feed and calm him by myself it felt like a super-power. I was attuned to his hunger and met his needs. I have always been attuned to my own hunger and rarely overate. If I did, I got a stomachache and felt stupid for overdoing it, but never beat myself up about. But there is no need to do so, as Alison quips, “You didn’t kick a puppy, you ate food.” I came to understand that many women (and some men) feel stupid, guilty and ashamed after every meal. If this is your experience, Alison provides incredible advice throughout this book and I am only sharing bits and pieced with you in this post. Alison and I talk more about how I developed my strong positive body image in a recent IG Live. Check it out HERE! Back to her book...My biggest take home was gratitude – have gratitude for your food and your body. At a young age teach kids to have gratitude for their bodies and their food. I think it helped me tremendously that I said grace after every meal growing up. And that my Dad shared that during and immediately after world war II they didn’t have enough food. I think that ingrained in me a sense of responsibility to myself and my health to eat properly to fuel my body’s needs and not over or under nourish.
The next nugget I gleaned was to connect. Connect with nature, with God (if you are religious), with your community, friends and family. Enjoy every moment and allow the serotonin to flow. In chapter 5 Alison discusses how a dopamine rush (from food) tends to be more exciting when you aren’t connecting with others and having meaningful relationships. So to avoid being manipulated by the rush of food, learn to eat and enjoy in a meaningful way. I also learned that the concept of “health” isn’t as cut and dry as one might think. When we see someone fit and trim we might immediately assume she or he is so healthy! But this may not be the case at all! I love her approach in chapter 7, reminding us to choose “growth mindset” language instead of a “fixed mindset.” For example, do you ever tell yourself: You’re either eating healthy or, you’re not? Black and white thinking, such as being good or bad, healthy or unhealthy, is a fixed mindset. A healthy eating mindset starts with the mindset that healthy eating is not about being perfect. It’s about making an effort each day. Its about process not perfection! Alison takes a very practical approach to helping her clients and readers. Some of the skills and tools she shares are from cognitive behavioral therapy, CBT (and mindfulness-based CBT, MBCT, specifically). Mindfulness is a state of being, where one is fully present in the moment and does not judge or react to their thoughts and emotions. The mindfulness practice that is emphasized in MBCT is mindfulness meditation. Mindfulness meditation is thought to help us understand that thoughts and emotions come and go and that "you are not your thoughts." For example, in Chapter 8, she introduces thought stopping and breathing techniques to help shift awareness from one’s Inner bully. This is incredibly useful when your inner bully is beating you up about your body - or anything else! At the end of the book, Alison reminds us that our bodies will always come back to our set points, and that fighting our biology is a stressful way to live! She mentions that pregnancy was a strong example of this for her because her body put on the weight she needed to grow her baby, and then lost around the same amount each time. I remember that pregnancy was the first time in my life that I never felt self-conscious about any outfit I chose. I felt amazing in everything I put on and let my baby bump show in all its glory! Even thought I had never been so big, I could trust that my brain and body would know what to do, as long as I didn’t let that inner bully guide the way! Overall, I really appreciated Alison’s tangible advice, with each chapter ending with “key takeaways,” affirmations and easy to practice exercises. I think this book is a lovely addition to any therapists’ bookshelf and would recommend it to my clients, whether they struggle with body image, or not. The Reproductive Psychology Program has been a professional goal of mine for a long time. My maternal grandparents were both physicians; My grandfather was an OBGYN and my grandmother was a pediatrician. In the 1980’s, at the height of their practice, they turned half of their large city apartment into an outpatient clinic. I remember going to visit and watching the women and new mothers come and go all day long. Some were pregnant, some had newborns, many had multiple children. These women mostly looked happy. Overwhelmed, perhaps, but happy. Some were crying. Some looked distressed. I wondered to myself, did anyone ask them how they are feeling? As I matured and noticed how the medical system worked (for myself personally, but also as I volunteered in hospital and clinics), I realized that care was very siloed. I thought that this was far from ideal for reproductive aged women. As I started to learn about psychology in my high school senior year elective and later volunteered at a Crisis Center, I considered how damaging this isolated medical care could be for new families. After college when I decided to pursue graduate school in clinical psychology and focus on women’s mental health, I was exposed to evidence from decades of research that everyone benefits from the integration of behavioral health and primary care services (like OBGYN) which improves patient care and outcomes.  In September 2019 I started seeing patients for individual cognitive behavioral therapy one day a week in my new Reproductive Psychology Clinic at Cedars Sinai. This clinic is integrated into the Prenatal Diagnostic Center at Cedars, where women at higher risk for adverse perinatal outcomes are seen by Maternal Fetal Medicine specialists. These women are also at highest risk for perinatal mood and anxiety disorders. I was a one woman show at first, but the first year showed us that many women need these services and the clinic has since grown!  I am delighted to be working with several excellent mental health providers: Dr. Sinmi Bamgbose, MD is our Reproductive Psychiatry Consultant, Caryn Lindsey, LCSW, is our licensed clinical social worker, group therapist and patient navigator and Megan Doyle, LCSW, facilitates our support groups (e.g. perinatal grief and loss). Although individual and group psychotherapy are only available to California residents, these support groups are open to women throughout the USA! Click HERE to read more about our services on our website and click HERE to read the full press release. Our goal is to reach pregnant and postpartum women with evidence-based psychological interventions as well as prevention through education, screening and early referral to care! When needed, our consultation psychiatrist works directly with our patients' medical providers (OBGYN) to make psychotropic medication recommendations. Patients and providers are invited to register for our FREE virtual open house. We have one every first Monday of the month at 4:30 PM Pacific time. Please click HERE for registration information. We are looking forward to meeting you soon! The Improving Outcomes Program is led by Maternal Mental Health Now and funded by LA Care and Cedars Community Benefit Giving Office. I am proud to serve as the Cedars site PI and our sister medical sites are Watts Healthcare and USC Eisner. The Improving Outcomes Program was created in 2017 in response to the gross disparities in adverse birth outcomes, including postpartum depression, experienced by Black women compared to other races. Maternal Mental Health Now is a local non-profit organization dedicated to removing barriers to the prevention, identification and treatment of perinatal mood and anxiety disorders in Los Angeles County. A major goal of the Improving Outcomes Program is to provide psychoeducation and support for pregnant black women, so they feel comfortable in their medical home before delivery. In partnership with iDREAM for Racial Health Equity this 4 session program, Safe and Sacred Pregnancy, will be peer-led, facilitated by Raena Granberry and Ellen Branch, who will provide communication tips and tools for women to use with their doctors, nurses and hospital staff as they navigate their pregnancy and birth experiences. MMH-NOW will be hosting these virtually, so please register HERE and help us spread the word about these support groups! Another major goal was to provide training on cultural humility in the medical setting in partnership with iDREAM for Racial Health Equity. We will be presenting our preliminary results from the five Cultural Humility training sessions offered at Cedars-Sinai at the Postpartum Support International Conference on Friday July 9th, 2021!
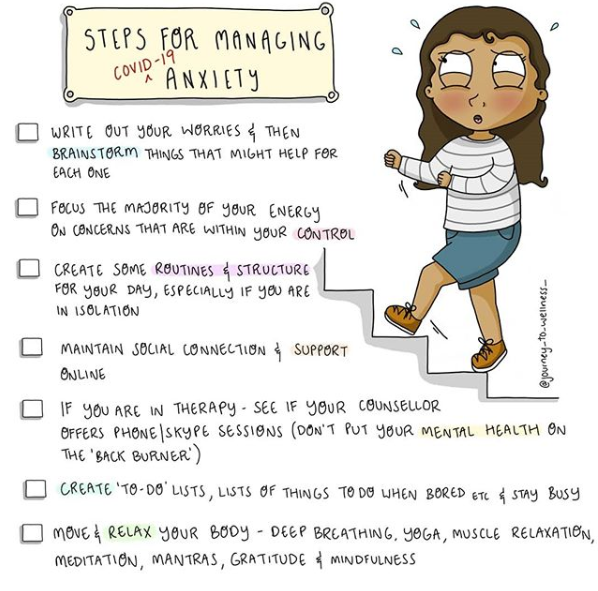
COVID-19 is a new virus and there is a never-ending stream of updates. The uncertainty about the virus and the changes that are rapidly unfolding no doubt make most of us feel on edge. This is normal, and mild anxiety can actually motivate us to take to take action to protect ourselves and others, and to learn more about the pandemic. That being said, we all like stability, routine, and a sense of control over our environments and experience tremendous stress when there are disruptions in our normal lives! COVID adds a new challenge for pregnant women, women delivering their babies and the postpartum period. All of these can be stressful times and 10-20% of women may develop a perinatal mood or anxiety disorder (PMAD) in the best of times, but COVID adds a very difficult layer. For example, adjusting to parenthood after delivery is challenging under normal circumstances, let alone in the midst of a global pandemic. Concerns about exposure to COVID-19, combined with physical distancing recommendations, can worsen depression and decrease access to the resources, such as health care and social supports, that women typically use to build resilience and promote recovery. Despite these challenges, there are several steps women with a perinatal mood or anxiety disorder can take to optimize their mental health and thrive in the face of COVID-19. 1. Prioritizing Self-Care: Remember the acronym R.E.S.T. (image below) and keep in mind that during these unique times self-care might include limiting/minimizing your media/news consumption and being creative about how you exercise: 2. Access Social Support: Related to Therapy, above, social support can be invaluable at this time - especially for women who have mild (not severe) symptoms of anxiety, depression or stress. However, COVID-19 presents unique barriers to engaging supports, particularly those outside of the home. Partners are a logical first choice, but if one is not present (or able), it may be helpful to seek outside help from family or friends. One silver lining in the COVID-19 cloud is that many restrictions on telehealth – particularly teletherapy and telepsychiatry – have been lifted. Many providers and support groups have quickly pivoted to offer meetings and therapy online. Here are some notable resources for women who are pregnant or new moms struggling with anxiety or depression: Postpartum Support International offers daily on-line support groups, links to local resources in all 50 states, and an online provider directory. The Bloom Foundation hosts virtual support groups. Maternal Mental Health Now has designed a new resource to help you feel prepared to adjust to the emotional demands, joys, and stressors of trying to conceive, pregnancy and parenting. They also partnered with Dignity Health to provide a series of virtual support groups: 3. Experience all of your emotions: Dr. Kessler who is the world’s foremost expert on grief was recently interviewed and suggested that we are currently experiencing several types of griefs (collective, anticipatory). All of the feelings that come along with this COVID-related grief are overwhelming and trying to stop them to avoid feeling sad or angry in our grief will not help. Kessler says: When you name it, you feel it and it moves through you. Emotions need motion. It’s important we acknowledge what we go through. One unfortunate byproduct of the self-help movement is we’re the first generation to have feelings about our feelings. We tell ourselves things like, I feel sad, but I shouldn’t feel that; other people have it worse. We can — we should — stop at the first feeling. I feel sad. Let me go for five minutes to feel sad." Give yourself permission to feel. Disappointment around creating a new birth plan? #Anxious about rescheduling your baby shower? Let those feelings move through you and move on. "Let yourself feel the grief and keep moving." 4. Radical Acceptance: Taking the approach of radical acceptance can be important when dealing with an overwhelming situation such as the current one. It is about recognizing and accepting the truth of the situation, even if it is difficult. It is also not burying our heads in the sand. For example, it is not continuing with our daily routine like nothing has changed. Many of our typical routines have changed substantially. It is recognizing what is and where we can act and respond accordingly. It is realizing what is out of our control, but also what is within our control. Some example of this for pregnant and postpartum women would be:
1. March of Dimes has created a wonderful resource for women to update their birth plan and realizing that what we plan may still not come to happen in COVID times. for this purpose: COVID UPDATED BIRTH PLAN. 2. Evidence Based Birth has high-quality online childbirth education classes. 3. LiveHealthOnline has online lactation and breastfeeding support. 4. National Domestic Violence Hotline helps women create a safety plan HERE. Updated 1/22/20 and 6/12/20 The Improving Outcomes Program is led by Maternal Mental Health Now and funded by LA Care and Cedars Community Benefit Giving Office. I am proud to serve as the Cedars site PI and our sister medical site is Watts Healthcare. The Improving Outcomes Program was created in response to the gross disparities in adverse birth outcomes, including postpartum depression, experienced by Black women compared to other races. Maternal Mental Health Now is a local non-profit organization dedicated to removing barriers to the prevention, identification and treatment of perinatal mood and anxiety disorders in Los Angeles County. A major goal of the Improving Outcomes Program is to provide training on cultural humility in the medical setting and a partnership with iDREAM for Racial Health Equity was the next logical step. Another important step is to provide psychoeducation and support for pregnant black women, so they feel comfortable in their medical home before delivery. This 5 session program will be facilitated by Black Women for Wellness, another local organization and will provide communication tips and tools for women to use with their doctors, nurses and hospital staff as they navigate their pregnancy and birth experiences. MMH-NOW will be hosting a series of support circles for pregnant black women at various locations across LA County throughout 2020. The Spring groups were canceled due to COVID-19 but new groups will take place this Summer/Fall, with updates ASAP. Each session is five weeks long and is facilitated by Raena Granberry. Please help us spread the word about these support groups!
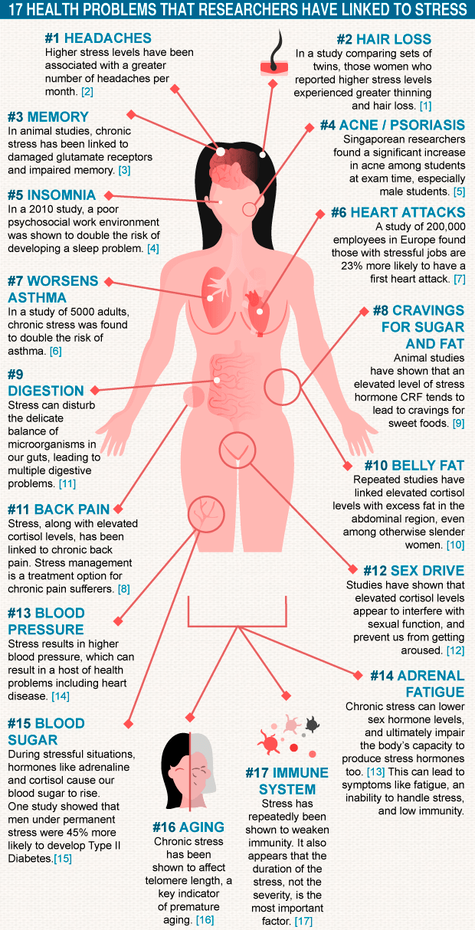
Our goal with both arms of this Program is to help change the trajectory of Black women’s maternal and reproductive health. Please check out this special edition of the new Tribune Media syndicated series ALLIES, below! Comedian and “Accidental Activist,” Angelina Spicer, describes her journey from despair to healing and then to advocacy. I am the voice of expertise in the piece, discussing postpartum depression (PPD) and the fact that African American women are 3X more likely to suffer from PPD. I also introduce the Improving Outcomes Program to share we can do in the hospital center setting! Click HERE for direct link to the Emmy Nominated (June 2020) ALLIES episode and image below to be directed to KTLA story. Women with adverse pregnancy outcomes such as hypertension, preeclampsia, diabetes, and preterm delivery are at significantly higher risk than women without these complications of developing early cardiovascular morbidity later in life. Depression is a neglected dimension of maternal morbidity and women with depression are 5 times as likely to progress from maternal morbidity (illness) to mortality (death). Depression is common, 8-13% of pregnant women are diagnosed with depression, and prenatal depression is associated with gestational diabetes, preeclampsia and low birth weight. A growing literature supports links between depression, anxiety and stress and cardiovascular disease (CVD) in older women. As you can see in #6, #10, #13, #15 and #17, all related to CVD below, it is important that women make efforts to reduce stress in their lives as early as possible! In order to provide clinical cardiovascular screening and preventive care to women who had an adverse pregnancy outcome, we instituted a Postpartum Heart Health Program in January 2015 within the Barbra Streisand Women’s Heart Center (BSWHC). The clinic is tailored to offer a comprehensive cardiovascular risk screening and risk stratification to patients who had an adverse pregnancy outcome. The purpose of the practice is to screen women with adverse pregnancy outcomes for CVD, teach them about cardiovascular health, stress reduction, and offer annual follow-up if desired.
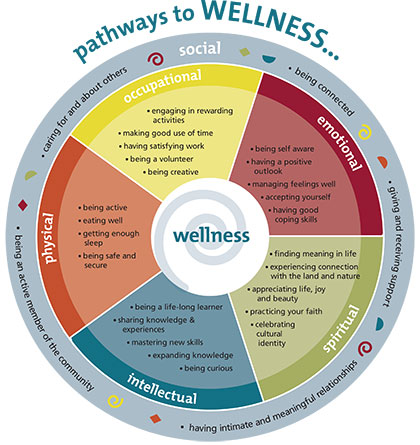
I always thought that “wellness” was just another way to say good mental health. Or if I wanted to consider physical health too, that it was the opposite of disease. Wellness is so much more! As you can see in this image, there are actually (at least) six dimensions of wellness, developed by Bill Hettler, MD, in 1976. This interdependent model describes a whole person approach to wellness. We often focus on the physical and emotional pathways but what encourages me is that we can improve our wellness on the other dimensions and have improvement trickle over! For example, when we take (drag) our kids hiking they eventually get lost in the beauty of our surrounding hills too. We can teach them all about nature while getting physical exercise, spiritually connect with the Earth and God's creatures (if you are religious) and spend quality time with our loved ones, and it all leads to an improvement in our mood and physical health. I encourage you to give yourself a Wellness Week! Take a few hours and focus on how you can improve your wellness on at least 3 of these dimensions this week. Simple steps like going for a walk with a friend can make significant changes to your health and well-being and improve your wellness on 2 dimensions at a time - physical and social! If you live locally in Los Angeles, please consider stopping by an upcoming Wellness fair (click HERE for link to registration website)! Perinatal Mental Health Care will be participating in this SocalMom Wellness event. Events like these allow me to improve my wellness on at least 4 dimensions at one time - social, intellectual, emotional and occupational! Hope to see you there!
Women are 2-3 times more likely to suffer with depression and anxiety in their lifetime than men. But rates are the SAME before puberty and after menopause! Reproductive mood and anxiety disorders have been my research and clinical interest since my first year in graduate school. I started out by investigating risk for premenstrual dysphoric disorder (PMDD). PMDD is a chronic condition that significantly affects well-being during the reproductive years. The pattern of symptoms of PMDD is linked to the menstrual cycle, with the onset of symptoms in the late luteal phase (2-3 days before a period begins) and the symptom offset shortly after the beginning of menses. At least five of 11 symptoms are necessary for diagnosis, with at least one of the symptoms being related to mood. Symptoms include depressed mood, anxiety/tension, affective lability (ups and downs), anger/irritability, decreased interest in activities, difficulty concentrating, fatigue, appetite changes, sleep difficulties, feeling out of control and physical symptoms. I found the most common emotional symptom reported was irritability. PMDD is associated with significant personal and economic costs, increased work absenteeism, reduced work productivity, and reduced quality of life. Sex differences in depression rates suggest that women might be at increased risk for psychiatric illnesses as a result of naturally changing hormonal levels during their reproductive cycle. In addition to high rates of pregnancy, postpartum, and perimenopausal depression, up to 85% of menstruating women exhibit one or more menstrual cycle related symptom, 20–40% report Premenstrual Syndrome (PMS), and 2–9% report PMDD. My current research focuses on inflammation driving the mood & anxiety symptoms that arise during naturally changing hormonal levels in pregnancy and postpartum. My early research focused on other biological risk factors, for example, I measured the electrical activity in college women's brains. This EEG research has been published and showed that women with PMDD have similar brain frontal brain activity as those with major depression - even if they are in the follicular phase of their cycle (ie. not having mood or anxiety symptoms)! I also published a diagnostic tool for PMDD researchers to use, since none existed in 2002-2005. Links to all of this research can be found in ResearchGate. If you have trouble accessing any articles, please let me know. I can send you a full PDF (for educational purposes only).
|
Dr. Accortt in the NewsAugust 2023: KPCC Radio AirTalk with Larry Mantle, FDA Approves Pill Designed To Work Faster For Postpartum Depression
August 2023: KABC TV: Postpartum depression drug aimed at prioritizing maternal health, especially in communities of color February 2023: Glamour Magazine: Postpartum Anxiety Is More Common Than You Think—Here’s What You Need to Know December 2022: Cedars-Sinai Newsroom: Immune System Irregularities Found in Women With Postpartum Mood & Anxiety Disorders October 2022: Verywell Family, Researchers Find Possible Predictor of Postpartum Depression June 2022: ABC News, Postpartum Depression Screening, Changes to Nurse Training. August 2021: AirTalk KPCC Radio, The History of C-Sections, The Significance We Put on "Birth Stories" And How It Impacts Mental health (fast forward to 13 minute mark) July 2021: AirTalk KPCC Radio, Why Women Have Long Kept Early Parts of Pregnancy a Secret and the Arguments For Moving Away From the 12-week rule (fast forward to 28 minute mark) July 2021: Los Angeles Times, Postpartum depression on the rise, especially for women of color, during COVID-19 pandemic October 2020: The Candidly, PMDD Affects Millions Of Women. So Why Aren’t We Talking About It? October 2020: Cedars-Sinai Discoveries Magazine, A Real-Life Stress Test September 2020: Cedars-Sinai Blog, Infertility and Mental Health July 2020: Cedars-Sinai Newsroom, Reproductive Psychology Program Focuses on Mother and Family Wellness May 2020: Hawaii News Now, Sunrise, How to Prevent Anxiety & Depression Before and After Giving Birth April 2020: The Bump, How to Spot Postpartum Depression in Your Partner or Friend 12/3/19: Quartz, Ten questions about mothers’ mental health could promote resilient pregnancies 5/10/19: CGTN America, US comedian uses her act to turn the spotlight on postpartum depression 5/1/19: KTLA News, How One Comedian’s Battle With Postpartum Depression Turned Laughs Into Legislation 3/20/19: KFI News Radio, FDA Approves First Drug for PPD, Brexanolone (Zulresso) Winter 2019: Cedars-Sinai Discoveries Magazine, Stop The Stigma 9/11/18: USC Center for Health Journalism, Cedars-Sinai PPD Screening Program May be Model for State Summer 2018: Cedars-Sinai Catalyst Magazine, The Helping Hand of Los Angeles Funds Postpartum Depression Screening Program, scroll down to page 40 of magazine 5/18/18: TODAY.com, Alyssa Milano on Postpartum Anxiety 5/3/18: Cedars-Sinai Maternal Mental Health Research 10/19/17: Cedars-Sinai Postpartum Depression Screening Program 3/24/17: MomCo. App for Social Support Blog Archives
May 2022
AuthorDr. Accortt is a California licensed clinical psychologist. When she isn't seeing patients in private practice she conducts research in the OBGYN department at Cedars-Sinai. She will update this page with important maternal mental health news and research. |




















 RSS Feed
RSS Feed